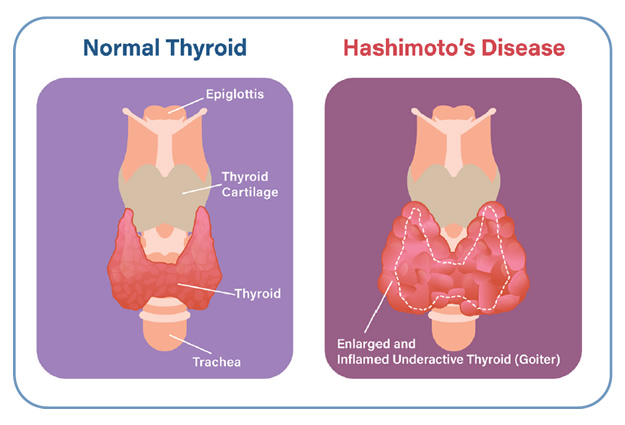
WHAT IS HASHIMOTO’S THYROIDITIS?
Hashimoto’s thyroiditis is also known as chronic lymphocytic thyroiditis or autoimmune thyroiditis. It is an autoimmune disorder. This means you develop antibodies [thyroid peroxidase (TPO) and/or thyroglobulin (Tg) antibodies] that damage your thyroid gland. These antibodies cause inflammation in your thyroid gland. Over time, the inflammation can cause your thyroid gland to
- get bigger (goiter).
- have trouble making enough thyroid hormone (hypothyroidism).
In the United States, Hashimoto’s thyroiditis is the most common cause of hypothyroidism.
- Hashimoto’s thyroiditis often runs in families.
- It occurs most commonly in women, but it can also affect men.
- It is more common as you get older but can occur at any age, including in children.